Even after three outbreaks and more than 300 cases, COVID-19 still not our greatest threat
April 6, 2021

The pandemic has been a challenge for the Calgary Drop-In Centre, there is no doubt about that.
In the early days of March 2020, we feared the worst. Would there be mass deaths among the vulnerable population and frontline staff? Would we have enough space for everyone needing shelter? Would we be able to keep stock of enough toilet paper and PPE? When we experienced our first positive cases in shelter, would an organization with more experience in managing outbreaks step in and take over?
During these past 12 months, we are grateful that no clients have lost their lives to COVID-19. Our maximum capacity has been reached only a handful of times, and our stock of supplies has been plentiful (with great thanks to our concerned and compassionate community). Alongside our peers, system planners, governments, and community, we learned how to handle outbreaks as if we were experts in pandemic response all along.
Housing-Focused Emergency Shelter
In fact, we attribute our recent housing outcomes to COVID-19. While everyone was asked to stay home, folks experiencing homelessness had nowhere else to go but shelters. In turn, the DI was able to garner more funding to be used for security deposits and other moving costs, support from landlords, and client readiness than any other year. To this end, we helped 428 people exit homelessness and find a home of their own in the 2020 calendar year – a 24% increase over our 2019 housing outcomes. Several of these recently housed folks were long-time, institutionalized shelter stayers who may not have had confidence that they could live independently before the pandemic hit.
Drug Crisis Escalating
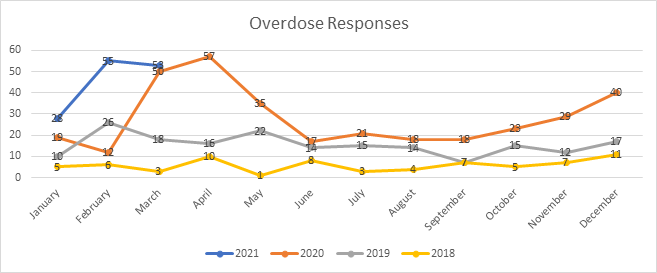
In contrast, many of the folks in shelter have significant and often unpredictable physical and mental health concerns, and as such, they are limited in their housing options. In fact, the most consequential part of the pandemic has not been COVID-19 at all. Rather, it has been the staggering number of overdoses that have taken place among folks in our care. Even though the number of people the DI can serve each day has been reduced by half due to COVID-19, people are overdosing at a higher rate than we’ve seen before.
Since the beginning of the pandemic, frontline staff at the DI have responded to 433 overdoses¹.
These numbers equate to more than one overdose each day, and it’s not uncommon for the same people to overdose again and again. In these first three months of 2021, we have responded to another 136 overdoses and within the same time period, there have been seven people who lost their lives after a suspected overdose despite our interventions².
What’s more, we are finding ourselves using an unprecedented amount of Naloxone, a medication used to block the effects of opioids. It’s taking an average of four — and as many as ten — doses of naloxone for folks to come to. To put this in perspective, our Naloxone kits come with three doses, so we are going through multiple kits to reverse one overdose.
Addiction is rooted in individual and intergenerational trauma, and COVID-19 has contributed to a spike in stressors, triggers, isolation, and pain. As people suffer – and this goes for all of us – we find mechanisms to cope with the pain. Some folks turn to pain killers such as opioids, which (albeit temporarily) take away the deep and agonizing pain of their trauma and reality.
A Delicate Balance
To be clear, illicit drugs are prohibited at the DI. We employ a complicated balance of low-barrier, trauma-informed, harm reduction, and housing-focused philosophies while still doing everything we can to promote the safety and wellbeing of all clients, staff, and visitors. For example, we conduct regular bag searches and also have an amnesty tote program where folks can leave any item in a secured tote, no questions asked. This way, they can have a spot to eat and sleep without having to rid of their belongings. The alternative is they leave the DI with their non-permitted belongings and risk using and overdosing alone in a public space – our goal is to keep people safe as we face this drug crisis.
Because illicit substances inevitably find their way in the building, despite our best efforts, frontline shelter workers and nurses are consistently challenged to keep people alive on an ongoing basis. At the same time, people are struggling and have nowhere else to turn. There simply aren’t enough accessible detox beds and appropriate treatment options available in our city and we speculate that the severe mental health consequences of the pandemic (particularly during the winter) have people turning to drugs to cope more than we’ve witnessed before.
“We have dead bodies lying in front of us and it’s become our job to bring them back to life,” says a crew supervisor.
Impact on Staff and Clients
One minute, frontline staff may be serving lunch, helping with medication, educating about the importance of wearing a mask, or talking about housing. The next minute, they’re performing their required 10-minute bathroom check not knowing – but certainly dreading – who they might find in a state of lethal ecstasy. “We have dead bodies lying in front of us and it’s become our job to bring them back to life,” said a crew supervisor. The trauma of these incidents should not be understated, and the impact on staff and clients has been significant.
For staff, sometimes, these incidents require them to tap out and take some well-deserved wellness time, unintentionally leaving crews with fewer staff for the rest of the shift. Other times, staff feel the pressure to be frontline heroes and leave their own psychological wounds unattended, putting their team and clients first.
For clients, they are experiencing the trauma of receiving Naloxone directly, or they’re witnessing their friends and comrades go through these medical emergencies regularly.
What’s Next?
As a housing-focused emergency shelter in the middle of a global and unprecedented pandemic, we aren’t in a position to have all the solutions to the drug crisis. At the very least, however, we can share our reality with decision-makers: the homeless population needs more immediate access to detox, rehabilitation, and mental health services. For example, we know that some people are inclined to get clean directly after they come back from a near-death overdose. Right now, as a frontline service, the best we can do is add those who are ready to a long waitlist.
The high number of overdoses during COVID-19 may suggest there aren’t easily accessible mental health services for low- and no-income people to work through their addiction or prevent addiction in the first place. Along with detox and rehabilitation services, the homeless-serving sector and those we serve also need access to professional mental health support to work through their trauma and learn how to maintain healthier coping mechanisms. That said, we are hopeful to learn more about initiatives like the Rapid Care Counselling pilot aimed at connecting folks in shelters with mental health supports best suited to their needs – programs like this are a critical first step and we look forward to seeing how it develops. We applaud the collaborative efforts of Calgary Homeless Foundation, CUPS, and Catholic Family Service who launched the pilot in February 2021. Learn more about the Rapid Care Counselling pilot here.
In the meantime, we will continue to respond and do our best to keep folks alive until we can support with housing or connecting to appropriate services.
Please, Be Kind
As for you, our dear friends, we ask for your continued kindness, compassion, and understanding when it comes to those struggling with mental health, isolation, and addiction. Everyone is coping the best they can with the tools and supports that are available to them. If you see someone at risk or in the process of overdosing in public, please call 911 to get them medical attention. You can also consider learning how to use Naloxone and carry it with you in case of an emergency. Learn more about Naloxone here.
Finally, if someone you know works in the homeless-serving sector, please check in on them and give them some love. It can be challenging to talk about, so acknowledgment and an offer of gratitude can go a long way.
“Be Kind, for everyone you meet is fighting a mighty battle.” – Plato
¹This data was pulled between the dates, March 11, 2020 (the day the pandemic was announced) and March 31, 2021.
²We do not receive cause of death information from the medical examiner, so we cannot make the claim these deaths were caused by their overdose.
Recent Posts
February 10, 2026
December 11, 2025





